Introduction
Sleep is one of the most fragile yet essential components of wilderness performance, underpinning physical recovery, cognitive clarity, and emotional resilience. In the backcountry, sleep quality is disrupted by altitude, environmental stress, gear limitations, and psychological arousal, making it a central systems problem within the Wilderness Systems Framework (Body, Mind, Environment, Gear). This report examines whether naturopathic sleep aids such as melatonin, theanine, glycine, magnesium, and select botanicals can serve as safe and effective levers to enhance restorative deep and REM sleep without the risks of prescription or over-the-counter drugs. Drawing on physiology, biochemistry, and current evidence, the discussion evaluates benefits, hazards, and limitations, and situates these agents within a practical decision-making framework. Ultimately, the case is made for judicious, problem-specific use: sleep aids are not shortcuts, but tools that (when integrated into a coherent wilderness system) may improve safety, recovery, and overall backcountry experience.
Table of Contents • Note: if this is a members-only article, some sections may only be available to Premium or Unlimited Members.
- Introduction
- Background and Context
- Sleep in the Context of the Wilderness Systems Framework (WSF)
- Backcountry Sleep Challenges
- What Constitutes Good vs. Bad Sleep?
- Deep vs. REM Sleep
- How Naturopathic Sleep Aids Work
- Risks, Hazards, and Limitations in Wilderness Use
- Benefits in the Backcountry Context
- Summary Table: Naturopathic Sleep Aids in the Backcountry
- Wilderness Systems Framework Mapping: Sleep Aids as System Levers
- Practical Framework for Backpackers
- Evidence Quality and Limitations
- Ethical and Philosophical Considerations
- Conclusion
- Appendix 1: Buying Naturopathic Sleep Supplements – Evidence, Risks, and Consumer Protection
- Appendix 2: Key References (Annotated)
- Related Content
Background and Context
Why Sleep Matters in the Backcountry: Recovery, Safety, Decision-Making
Sleep is a primary driver of recovery in wilderness environments. Deep sleep stages support muscle repair, immune function, and metabolic regulation – processes that determine whether the body can sustain repeated days of exertion under load. Inadequate recovery leads to a progressive erosion of physiological capacity.
Cognitive performance is equally sleep-dependent. REM sleep, in particular, underpins memory consolidation and decision quality. Sleep restriction and fragmentation increase reaction times, reduce situational awareness, and amplify cognitive biases. In a backcountry setting, where navigation, responses to the environment, and analysis of objective hazards demand precision, these impairments translate directly into elevated risk.
Safety outcomes emerge from this interplay. Sleep loss increases the probability of acute accidents (e.g., falls or navigation errors) and chronic stress-related breakdowns (e.g., overuse injuries or illness). Fatigue also undermines crisis response and group cohesion.
In short, sleep is not just a luxury in the backcountry, but a systems-level determinant of wilderness performance and safety.

Sleep Disruptors in the Backcountry
Backcountry sleep is constrained by a set of environmental, psychological, and material factors that distinguish it from frontcountry or clinical conditions, including altitude, anxiety, environmental stressors, and inadequate gear.
Altitude exerts a direct effect on sleep architecture. Hypoxia suppresses REM sleep, increases sleep fragmentation, and promotes periodic breathing. The net effect is reduced restorative capacity at elevations where metabolic and cognitive demands are already elevated.
Anxiety – whether resulting from wildlife concerns, storm exposure, or the social and psychological stress of isolation – activates sympathetic pathways that delay sleep onset and reduce total sleep efficiency. Even when duration is adequate, quality is often compromised by rumination and arousals.
Environmental stressors such as temperature variability, wind, precipitation, wildlife, and hostile terrain further degrade sleep continuity. Cold exposure increases metabolic cost, while heat disrupts thermoregulatory cooling essential for initiating deeper stages of sleep. Noise and tactile discomfort (uneven ground, slope, crowded campsites) contribute to repeated micro-arousals.
Inadequate gear compounds these effects. A poorly insulated sleep system, insufficient clothing, or minimalist shelter design reduces the capacity to buffer environmental variability. The result is an increased reliance on physiological reserves to maintain comfort and survival thresholds, which in turn further degrades recovery.
Together, these disruptors frame the wilderness sleep problem: sleep quality is seldom determined by a single variable but by the interaction of physiological stress, psychological state, environmental exposure, and the limitations of gear systems.
Framing the Question
The persistent challenge of achieving restorative sleep in the backcountry raises the question of whether pharmacological interventions can improve outcomes. Prescription hypnotics and over-the-counter sedatives are effective for inducing sleep but carry substantial liabilities in wilderness contexts: altered sleep architecture, cognitive and motor impairment, dependency potential, and safety hazards.
Naturopathic compounds such as melatonin, L-theanine, glycine, magnesium, and botanical extracts are widely available, generally considered lower-risk, and have emerging evidence for their ability to improve aspects of sleep quality without the profound side-effect profiles of conventional drugs. The critical question, however, is not simply whether these aids “work,” but how they affect the broader wilderness system: physiological recovery, decision quality, interaction with environmental stressors, and the function of gear systems.
This article examines the potential role of naturopathic sleep aids in the backcountry, with attention to both benefits and hazards. The goal is not to promote their use uncritically, but to evaluate whether they can be deployed safely and effectively as part of an integrated wilderness systems strategy.
Naturopathic vs. Prescription vs. OTC Sleep Aids in the Backcountry
Backcountry travelers may confront the practical question of whether to carry pharmacological sleep aids, rely on over-the-counter (OTC) remedies, or use naturopathic compounds. While all three categories may facilitate sleep, they differ markedly in their mechanisms, side-effect profiles, and operational implications in wilderness contexts. This comparison underscores why a focus on naturopathic approaches is warranted in the wilderness context:
- Safety in the field. Prescription hypnotics (e.g., zolpidem, benzodiazepines) and antihistamine-based sedatives (e.g., diphenhydramine, doxylamine) induce sedation but also impair balance, coordination, and reaction time. Morning grogginess is common and can increase the likelihood of cognitive and biomechanical impairment.
- Sleep architecture. Many pharmaceutical agents alter sleep stage distribution, typically by suppressing REM or deep slow-wave sleep. The short-term effect may be longer sleep duration, but the long-term cost is reduced restorative value – the very functions most needed under wilderness stress.
- Dependency and tolerance. Regular use of prescription sleep drugs carries risks of habituation, rebound insomnia, or withdrawal syndromes. These patterns are incompatible with the self-sufficiency required on extended trips where medical oversight is absent.
- Side-effect profile. Anticholinergic effects – dry mouth, dehydration, urinary retention, and constipation – are problematic in wilderness environments where hydration and elimination are already challenged. Other adverse outcomes include parasomnias (e.g., sleepwalking) and disorientation.
- Ethos and accessibility. Naturopathic compounds, in contrast, are widely available, generally lower in risk, and align more closely with ultralight philosophy. They can be carried in lightweight form, used without prescription, and integrated into a systems-based approach that emphasizes self-sufficiency and minimal hazard load.
| Category | Common Examples | Mechanisms | Key Benefits | Major Risks / Hazards | Field Suitability |
|---|---|---|---|---|---|
| Prescription (Hypnotics, Benzodiazepines, Z-drugs) | Zolpidem, Eszopiclone, Temazepam | Potent GABA agonism; sedative-hypnotic action | Reliable sleep induction/maintenance; rapid onset | Sedation, balance impairment, memory issues, REM/deep sleep suppression, dependency | Low: high safety risks in wilderness |
| OTC (Antihistamines) | Diphenhydramine, Doxylamine | H1 receptor antagonism; anticholinergic effects | Widely available; strong sedation | Morning grogginess, dehydration, urinary retention, impaired thermoregulation, REM suppression | Low-Moderate: side-effects compromise safety |
| Naturopathic | Melatonin, Theanine, Glycine, Magnesium, Valerian, Chamomile | Circadian entrainment, autonomic modulation, neurotransmitter balance, mild GABAergic activity | Mild sleep latency reduction, improved recovery, lower dependency risk, anxiety reduction | Variable response, possible GI upset, mild architecture shifts, interaction risks | Moderate-High: safer, but still requires pre-trip testing |
Prescription and OTC drugs may offer more immediate potency but introduce safety and system hazards that are amplified in the backcountry. Naturopathic agents, though less reliable, generally maintain a safer profile and align more closely with self-sufficient wilderness practice – provided their risks are understood and managed.
Sleep in the Context of the Wilderness Systems Framework (WSF)
The Wilderness Systems Framework (WSF) is my pedagogical model that organizes wilderness practice into four interdependent pillars: Body, Mind, Environment, and Gear. It’s been the foundation of my instructional design for more than two decades, and I’ve since used it as a tool to frame trip planning and preparation guidelines as well as expedition debrief and critical (emergency) incident analyses for search and rescue.
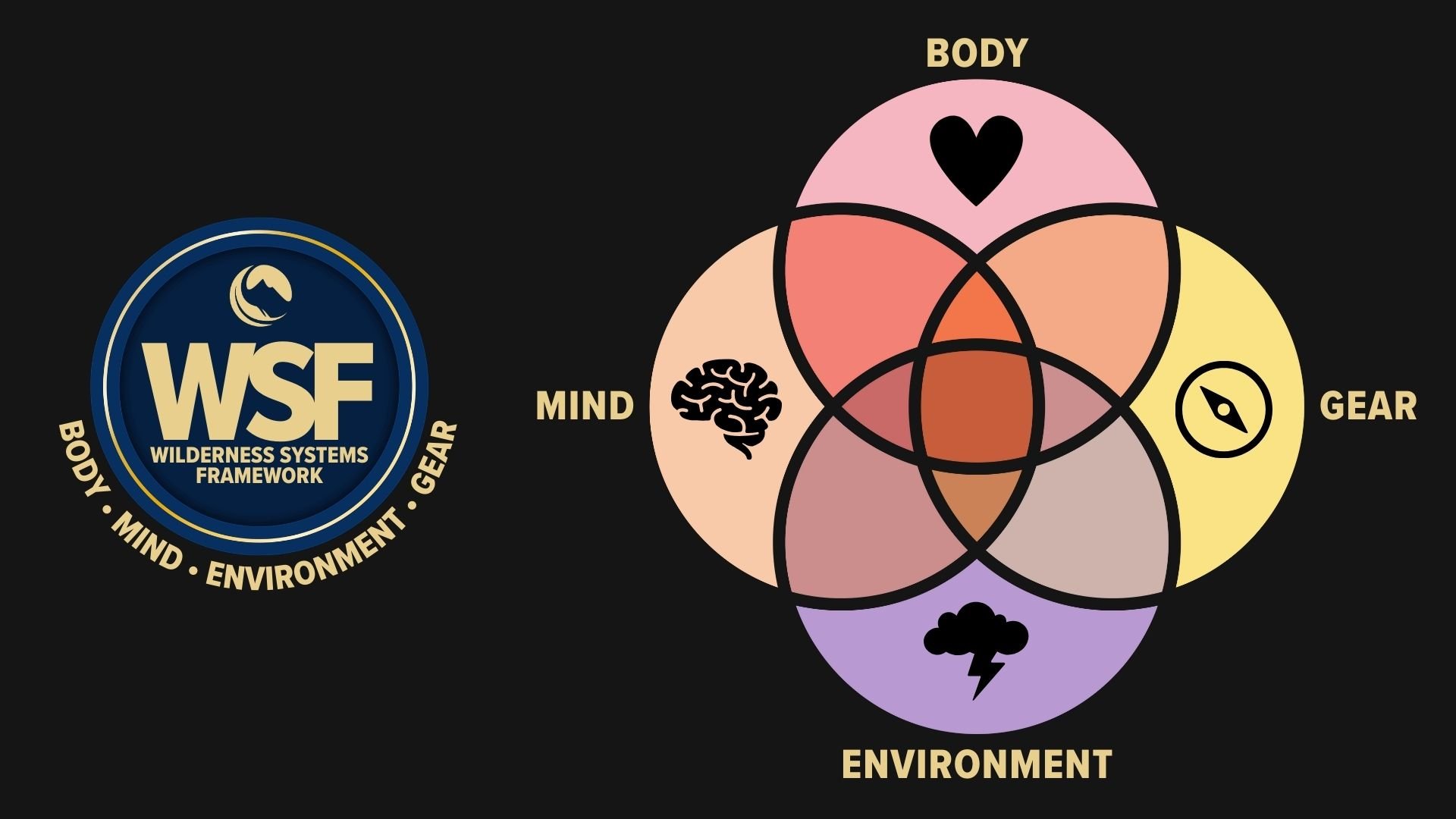
WSF emphasizes that safety, efficiency, and experiential quality emerge from their interaction rather than from any pillar in isolation. Sleep is a keystone process within this framework. It is not simply one variable among many, but a systemic regulator that influences physiology, cognition, environmental adaptation, and the function of equipment systems.
Positioning sleep within the WSF allows us to see it not only as an outcome (whether one “sleeps well” or not), but also as a driver of system-level performance. When recovery is adequate, the four pillars are balanced and reinforce one another. When sleep is disrupted, the imbalance cascades outward: physical fatigue undermines decision-making, cognitive impairment magnifies environmental risk, and insufficient recovery increases reliance on gear systems.
In this section, I will examine how sleep interacts with each pillar of the WSF and why its influence is best understood through a systems lens rather than as an isolated biological function.
Body
Sleep governs physiological recovery. Deep slow-wave sleep facilitates muscle repair, glycogen restoration, and immune regulation. REM sleep contributes to hormonal balance and thermoregulation. When sleep is insufficient, resting heart rate increases, heart rate variability decreases, and endurance capacity erodes. In the backcountry, this degradation manifests as reduced resilience to cold, altitude, and sustained exertion.
Mind
Cognitive performance is closely linked to sleep, particularly REM. Decision quality, bias recognition, and memory consolidation all depend on adequate sleep architecture. Sleep restriction increases reaction times, reduces situational awareness, and amplifies cognitive distortions. In wilderness contexts, where hazard evaluation and crisis response must be precise, these impairments directly increase risk.
Environment
The environment is both a source of sleep disruption and a multiplier of its consequences. Altitude suppresses REM and introduces periodic breathing. Cold and heat extremes disrupt thermoregulatory pathways critical to sleep initiation and maintenance. Wind, precipitation, terrain irregularities, and wildlife exposure further fragment sleep. Inadequate sleep in these contexts compounds physiological and psychological vulnerability.
Gear
Gear functions as the buffer between the individual and the environment, and sleep systems are the most direct example of this mediation. The system that includes your shelter, sleeping bag (or quilt), sleeping pad, pillow, and sleep clothing sets the baseline for comfort and recovery. When these systems fall short, hikers may rely more heavily on physiological reserves (or consider pharmacological supplementation) to compensate. In this sense, naturopathic sleep aids can be viewed as “pharmacological gear”: lightweight, portable interventions that extend or stabilize recovery capacity when environmental conditions or gear limitations reduce sleep quality.

Systems Perspective
Sleep integrates all four pillars. It restores the body, stabilizes the mind, moderates interactions with the environment, and defines the performance envelope of gear. When sleep is sufficient, these pillars reinforce one another and move the wilderness traveler closer to an optimal state of balance in the wilderness (defined by the Venn diagram’s intersection of body, mind, environment, and gear). When sleep fails, the imbalance cascades, reducing safety margins across the system.
Member Exclusive
A Premium or Unlimited Membership* is required to view the rest of this article.
* A Basic Membership is required to view Member Q&A events




Discussion
Become a member to post in the forums.
Companion forum thread to: Naturopathic Sleep Aids for Backcountry Use
Enhance performance and recovery in the backcountry through naturopathic sleep aids including melatonin, theanine, glycine, magnesium & botanicals.
I’m not a fan of anything that mutes my senses in the backcountry. I’ve had to wake up to deal with minor issues a few times, and it’s best to be clear-headed when that happens.
Recently I had some serious condensation in my DCF tent. If I hadn’t noticed and opened the vent, I would’ve woken up wet and freezing.
Oddly, while I don’t sleep easily at home, I sleep incredibly well when backpacking. It’s a different kind of sleep—just three or four hours at a time, roll over and repeat.
Interesting article. I don’t agree with the emphasis on naturopathic however. In addition to the fact that manufacturers don’t have to do rigorous testing but can make all kinds of claims for their products, I don’t think there’s anything inherently better about them over “mainstream” products. I also find that a Tylenol and an aspirin taken at mealtime can ease the aches and pains that can keep me awake, with no downside. I take them only as needed, so it’s not a crutch I rely on. A Benadryl is great for getting to sleep but I will have a hangover if I don’t take it early enough. Melatonin however, is awful for me. While it helps me fall asleep, I then wake up over and over again all night, and in the morning have such a terrible hangover, even including the headache! On melatonin I’m then groggy throughout the day, nodding off after lunch, or late in the afternoon. Then completely messed up for the next night.
The points about gear are well taken. Being warm and relaxed enough are essential for sleep, which is why I haven’t switched to a quilt; I want to be fully wrapped in warmth and have it roll with me when I turn over. I don’t really need much of a pillow; my clothes in a stuff sack with a fleece cover is adequate. Usually I’ve hiked hard enough that it’s all I need to get a good night’s rest.
One item not covered is a defensive device of some sort, which some of us do feel the need for, especially in some parts of America. I won’t sleep well if I don’t have something with me to fight back with – I’ll leave the discussion of what tool to carry to another thread. But I do have peace of mind if I am prepared. When you have the lifetime of experience of harassment, actual assaults, and on-going threats, you do what you have to do to stay safe.
<p>I used to take Benedryl. I also used to get leg cramps during the night. I stopped taking Benedryl and the leg cramps stopped, but I never correlated the two. Then I took Benedryl on one trip and the worst leg cramp of my life. I thought to myself, “Huh.” This doesn’t mean Benedryl causes leg cramps, but since I don’t take it any longer, I’ve had zero issues with nightly leg cramps. Anyone else had this issue?</p>
This used to be a thing, but the industry is pretty well evolved past this now. Lots of independent certification bodies (NSF, etc.) now exist to ensure quality and concentration. A little homework can ensure you are getting quality products.
These are known side effects of melatonin. Common with too high a dose (overwhelming the liver enzymes responsible for breakdown – and the effectiveness of these enzymes may be genetically-driven). So, take the dose where you experienced this and keep cutting it in half until the symptoms go away. Many users find positive effects from melatonin at doses as low as 0.2 to 0.5 mg. Most melatonin supplements seem to be in the 1g to 5g+ range.
The other issue is that if you are trying to resolve a sleep problem that is *not* related to circadian disruption, melatonin may compound the problem. For regular use, melatonin should be used to complement otherwise low melatonin in your body, resulting from disrupted circadian rhythms. Otherwise, you risk further disruption.
Biologically, downsides are not on-off switches; they lie on a spectrum that depends on individual dose, acute repetitive use, and chronic repetitive use. Less downside for lower dose and lower frequency of use. More downside for higher dose and higher frequency use. Again, downsides will be a function of a user’s individual biology.
Experiment, experiment, experiment. And consider context. Everyone’s biology is (a little bit) different.
Also, ignore manufacturer claims. Just focus on the chemistry.
Super interesting observation. I couldn’t find anything that specifically ties muscle cramps to Benadryl use, but Benadry is an anticholinergic (inhibits neurotransmitter function, part of its sedative strategy), so maybe there’s something there triggering leg cramps as a result of that mechanism of action…
NSF will verify that a drug is the amount advertised, but they don’t verify that a drug is effective.
I have problems sleeping. My sleep apnea doctor said none of the drugs are effective. Instead, go to bed at the same time every day. Do boring things for a couple hours before bed. Avoid bright or blue light 1.5 hours before bed. Look at bright lights when you first get up. Which might not be all that applicable to backpacking.
I tried melatonin. I think it was 1/4 of a 1g pill. No effect for a couple nights, then, the third night I couldn’t sleep at all.
I think melatonin would be good for jet lag, but not for regular sleep problems.
Thoughtful and thought provoking. I’m going to be re-evaluating my field sleep now! Thanks!
There are tools *other than drugs* that can be used to manage sleep problems (e.g., lifestyle and circadian rhythm behaviors, as you already mentioned), but this type of statement from a medical professional reflects broader issues from medical practitioners (especially specialists) in our modern-day healthcare system. Lack of critical thinking and failure to recognize all of these things as possible tools with relevance in certain contexts, seems medically irresponsible to me.
Winding down for a few hours before going to bed has had a profound impact on my sleep quality in recent years. +1
In a hiking context, that has motivated me to start hiking earlier, enjoying more quiet time in the early morning sunshine during my first break, and ending my day a little earlier so I can relax in camp before going to bed. I don’t do this every day, but on long trips I definitely try to pepper in this type of day every few days to take a break from dawn-to-dusk hiking.
At home, melatonin works well when my sleep times are irregular. While backpacking, it also works when I’m too over tired to get to sleep.
Taking too much makes the next morning feel like trash. Finding the right dose is important.
Melatonin in a proper dose lengthens REM and gives me wild and vivid dreams that worried me at first but that I’ve since learned to embrace and look forward to
Excuse me while I kiss the sky, thank you melatonin
My sleep apnea doctor said that the only effective treatment for insomnia is CBT-I. That’s where you go to a therapist and talk. cognitive behavior therapy insomnia.
There’s a website that talks about cbt-i. They say it augments cbt-i with a human. I got an idea what cbt-i is based on this. I would have gone to talk to a human but it was during covid shutdowns so I didn’t bother. https://mobile.va.gov/app/cbt-i-coach
This is more general than back country use, but I think it would help with that also.
Does CBD count as a botanical extract? seems to block or interfere with the inflammatory impulse which can help with sore muscles. Not sure if it has a calming effect exactly and here’s what google A-I reports:
CBD is not considered a mild sedative in the traditional sense, as it does not cause sleepiness or incapacitation. Instead of knocking you out, CBD promotes relaxation and can help calm the nervous system, which may lead to improved sleep quality. It’s important to distinguish CBD from its psychoactive counterpart, THC, and be aware that certain combinations of CBD with other sedating medications or substances could increase drowsiness.
Like Jay above not sure I want to be sedated in the backcountry but relaxed is OK. Also sometimes take a third (sliced by pill cutter so not precise) of a cetirizine AKA Zyrtec antihistamine to blunt allergic reactions. A-I says: Plus Side. Causes less sedation than older allergy medicines, like Benadryl. It is long-acting and lasts up to 24 hours.
Downside. Doesn’t control allergy symptoms as well as older allergy medicines. Use cetirizine mainly if drowsiness from Benadryl interferes with function.
I’ve noticed somewhat deeper sleep but like avoiding anti-histamine effects during waking hours so the light dose at bedtime. Seem to wake up just as easily and no grogginess. Usually a pollen season problem and added to pack in pollen season like rabbit-bush in the 4-corners about now.
IMO, one should be very careful in using naturopathic/alternative treatments. While some of them may be safe and effective, many are pure snake oil scams, and some are probably not safe at the doses some people may use them. Certainly, they are not generally evaluated for safety and efficacy to the same extent as pharmaceuticals, so one would really have to do one’s own due diligence to evaluate the scientific rigor of the “studies” that the manufacturer is claiming. And frankly, the vast majority of people are not really capable of distinguishing a legit study from one that is flawed. Moreover, there are important subtleties, like potential drug interactions, that may not be disclosed for supplements and remedies.
The placebo effect is real, and sometimes pretty strong, so you may get a benefit from something even if it’s not really effective. But history is rife with reports of remedies that are not safe … so be careful. When I see some of the people who are often making a lot of money promoting naturopathic or “alternative” remedies (e.g. Dr. Oz), that often tells me all I need to know.
Good points, Dan. Gotta have the data to back up the claims.
My frustration with the wellness industry is the intereptation that “a compound” isolated from “plant X” or whatever “does this thing” – which it does in controlled studies at a dose that’s completely irrelevant to the dose found in the supplement. For this article, I focused my energy on supplements that had a large body of evidence in peer-reviewed medical research, without placebo effects, and with measurable outcomes.
Also, FWIW, pharmaceutical sleep aids, while very successful at “putting your into a sleep state” have some pretty risky long-term outcomes that are largely absent with naturopathic sleep aids – dependency, tolerance, rebound, cognitive impairment, dementia risk (correlation studies), dexterity and coordination impairment, other symptom masking, depression/anxiety (due to how they affect brain function), and immunological impairment. Bioidenticals or endogenous supplements (e.g., melatonin and glycine) and bio-analogous compounds (e.g., theanine) or macronutrient minerals (e.g., magnesium), in particular, have been deeply studied and their risks are low when compared to the laundry list of risks associated with pharmaceutical sleep supplements.
The 2010s started sort of a golden age of pharma research, because a lot of the long-term data started coming in from the first big wave of pharma dev that started in the 1980s, and has started waking up the medical community to some of the long-term risks of putting things in our body just because the FDA said it was ok to so at some point in the past.
So maybe instead (or also):
The ship has sailed on most Americans (not sure about Europeans and others) fully believing and embracing unscientific solutions to health problems. Ivermectin cocktail anyone? If we’re taking health care advice from an uncredentialed heroin addict with a brain worm who has turned orange, there isn’t much hope for critical thinking. Measles party perhaps?
As a librarian, I’d also state from experience that many of the “peer reviewed” studies – even those that show up in Medline – are actually predatory journals. It’s a huge problem for science, one that undermines genuine work that could be helpful to many, if more actual unbiased research were funded. But as naturopathy stands, it’s not a legitimate field. Ryan if you want to convince folks about specific options, maybe disconnecting from that business model and focusing on those actual studies would be helpful.
100%. This industry has so many structural problems, including the funding of predatory studies, that it’s often very difficult to sort out.
Again, it always has to go back to data derived from independent studies with no funding conflicts of interest.
Grow your own.
Become a member to post in the forums.